Organizations globally are increasingly investing in workplace health and wellness programs. It’s no mystery why. The post-COVID-19 labor market has given workers far more bargaining power than in years past, creating intense competition amongst employers to attract top talent and to keep the talent they already have.
Interestingly, access to health and wellness services is quickly rising on the list of better workplace conditions demanded by employees. According to a 2020 study conducted by Morneau Shepell, 60% of employees reported that they would leave their current employer for another who provides better health and wellbeing support, even if they were offered less salary1.
But beyond the drive to attract and retain employees, investing in workplace health and wellness just makes good business sense. The National Business Group on Health reports that workplace wellness programs net anywhere between $1.50 and $3.92 return on every dollar invested, principally through the reduction of health-related absenteeism, lower employer health insurance premiums, and covered medical expenses, not to mention improvements in culture and worker productivity2.
It’s no wonder why U.S. employers spend an average of $3.6 million per year on these programs3. And yet, despite the considerable investments made, median employee participation rates in such workplace health and wellness programs rarely exceed 25%4. What’s going on here?
Below, we’ve highlighted some of the challenges organizations face in building greater workforce participation in their health and wellness initiatives. We’ll also offer some suggestions as to how companies can overcome these challenges, and specifically how they can leverage software to help them boost employee engagement levels with respect to workplace health.
Make Participation in Health Easier
One reason engagement levels in health and wellness programs are so low might have something to do with convenience. Research has revealed that over 7 in 10 employees decline to participate in workplace wellness initiatives – from voluntary health assessments to biometric screening to vaccination campaigns – simply because they find it too difficult to access services or can’t find the time to attend at work clinics5. Yet, according to Hero Health, employee participation rates in wellness programs rise between 5% to 10% simply when these services are made available through digital solutions6.
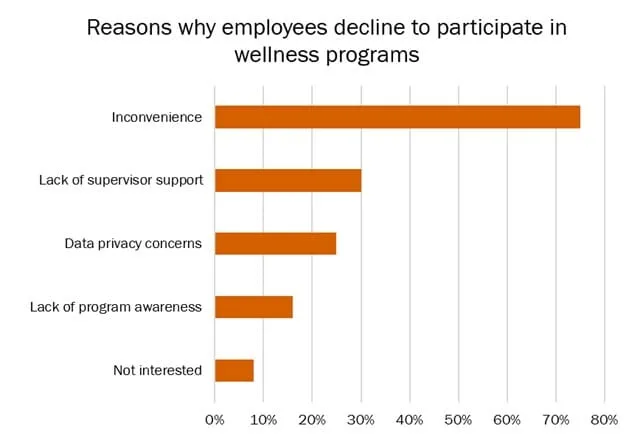
Source: Adapted from HealthMine5
EHS software is making it easier than ever to open up accessibility to workplace-based preventive health services. Mobile apps now allow employees to self-schedule their own wellness clinic appointments, affording users the ability to select their preferred date, time, clinic, and even health practitioner. Self-scheduling is one of the simplest steps toward removing barriers to participation. Moreover, mobile-enabled health programs make it easier for firms to offer a more personalized care experience to their workforce. Employees can complete health assessments, provide their health history, or even submit documentation right from their devices in advance of in-person appointments. This flexibility enables health professionals to align services more efficiently to specific employee needs while reducing overall time in the clinic. EHS platforms are even expanding their telehealth capabilities, enabling employees to seek care wherever they are, liaising with clinicians virtually, and removing yet another barrier to accessing high-quality, preventive care.
Improve Health Data Visibility
The rapid expansion of health-based software has led to what’s being called the ‘quantified self’ – the state in which individuals can track their physiological, behaviors, and other health indicators in real-time with technology, including mobile apps and wearables. But this growing trend raises an interesting question. Does the use of these technologies actually result in tangible improvements in personal health outcomes?
Recently, a team at New York University set out to answer this question. They conducted a 15-month randomized experiment to see whether health technology actually persuaded users to change their behaviors and lifestyles in a manner that actually lowered their personal health risk factors7. They found that the adoption of technology resulted in improvements not only to short-term health metrics (such as blood glucose levels) but to longer-term measures as well, including the frequency of hospital visits per year and total annualized health care spending. What explains these results?
If someone is in good health, there’s little impetus to visit a doctor. In fact, the uptake in preventive care is often correlated to an individual’s visibility to data on their personal health risk factors. Without that data, there’s really no “push” to encourage them to seek care, since overt signs of illness aren’t present. But we all know that illnesses can have long latency periods, where symptoms only appear after years of exposure to health hazards, at which point the resulting illness may have advanced significantly, resulting in worse prognoses, longer treatment periods, and overall increases in medical expenses.
And that’s why these technologies are so valuable. They empower the individual with actionable real-time data that can be used to inform their lifestyle choices and encourage them to seek out preventive care, to catch and address health risks before they grow into bigger problems. At Cority, we’re looking to expand employee access to such real-time health data. Clients utilizing our Occupational Health Solution have access to our Wellness Indicators feature – a series of health-related metrics linked directly to each user’s electronic medical record. Every time the employee seeks care within their company’s health and wellness program, key health metrics – like BMI, cholesterol levels, or even audiometric results – are accessible to them, quickly and securely, right on their mobile device. With Wellness Indicators, employees can monitor their personal wellness metrics in real-time, or even share this data with their external health providers, helping to inform treatment options and even creating a “spark” that might be enough to encourage behavioral changes that can lower their specific health risks.
Give Workers Ownership in Managing Their Health Risks
Let’s be honest. Getting a person to change their behavior requires a willingness on their part to want to change. And the best way to encourage behavior change is to put the individual in the driver’s seat– getting them to recognize the need to change and giving them the autonomy and support needed to make that change. This includes getting them actively involved in the process to identify and evaluate how their behaviors, decisions, and lifestyle choices can increase or decrease their health risks and potential for occupational injury and illness.
Unfortunately, many organizations rely on management-driven processes that limit employee engagement in the detection, evaluation, and control of health-related risks. And that lack of engagement often creates a resistance to change. But, if we were able to make risk data more relevant or “personal” to each individual, we might be able to encourage greater employee involvement in managing risk and empower individuals to address their behaviors and environments on their own in a way that promotes better health. This would, in turn, allow the company to focus its limited expert resources on the most complex, high-risk issues across its operating footprint.
The growth of remote and hybrid work provides a great test case for this novel approach to employee-led health risk management. In the rush to maintain business continuity at the outset of the COVID-19 pandemic, workstation design for remote-working employees wasn’t top-of-mind for many businesses. And the effects were immediately visible. In a survey conducted by Hinge Health in late 2020, 54% of remote employees reported that they were experiencing more pain in their back, shoulders, neck, and wrists than when they were working at the office8. Moreover, companies were left to contemplate how to manage risk in this new work environment in which they had limited visibility and control.
As remote and hybrid working models appear here to stay, organizations must now consider how to better enable their employees to identify and evaluate the risks posed by their environments and behaviors wherever they work and determine how to guide these employees to effectively manage these health risks without outside assistance. Fortunately, new tools are entering the market to support businesses facing this new front in health risk management, specifically by:
- Enabling risk self-assessment and self-management – These solutions allow employees to evaluate how their decisions, actions, and choices influence their personal risk level, and then empower them with prescribed recommendations and action plans, tailored to their unique risk profile, on what simple changes can be made to lower associated health risks. This might include workstation adjustments, on-the-job training, or access to health and wellness supports.
- Providing real-time behavioral data – Just because you have an ergonomically-designed workstation doesn’t mean you’ll never slouch at your desk. Just because you have a mask on doesn’t mean you wear it properly. Managing health risk effectively requires employees to continuously re-assess their behavior in real-time, and make slight adjustments. Solutions that provide this real-time behavioral data can help promote greater personal responsibility while reinforcing that the employee has agency over their risk exposure.
- Offering opportunities to build risk competency – Empowering workers to take a leading role in managing their personal health risks is dependent on building their risk competence – their ability to recognize and understand where risk exists, and its impact on their health and wellness. Employees need to be afforded continuous opportunities to develop new skills and strengthen knowledge for detecting and managing the health risks they face. New solutions are emerging to provide workers not only with better access to EHS learning, but offering them more control over when, where, and how they learn. By making EHS training available through digital platforms, organizations were found to improve access, boost knowledge retention up to 60% versus conventional methods9, and accommodate specific learning and literacy needs that can boost overall employee engagement.
Final Thoughts
In 2019, 73% of employees surveyed at organizations across 28 U.S. cities cited that a company’s health and wellness programs would influence their decision to consider a position10. That percentage is surely set to increase. But bringing a horse to water doesn’t mean it will drink. While more attractive health and wellness programs might help your business attract the best-of-the-best, organizations need to consider how to boost engagement in these programs to truly realize the productivity, profitability, and cultural benefits they can provide.
As the scope of the workplace continues to change and employees demand more choice and a more personalized experience at work, digital platforms offer businesses new ways to engage their workforce in their health and wellness initiatives, leading to healthier people and a healthier bottom line.
Sources
- Hussain, Y. January 28, 2020. ‘Posthaste: Canadians are financially stressed but would switch to a lower paying job in a heartbeat for this one perk.’ Financial Post. Accessed at: https://financialpost.com/executive/posthaste-canadians-are-financially-stressed-but-they-will-switch-to-a-lower-paying-job-in-a-heartbeat-for-this-one-perk
- Mattke, S. et al. 2014. ‘Workplace wellness programs: Services offered, participation and incentives.’ Rand Corporation.
- J. Kent. 2019. ‘Large employers to average $3.6M on wellness programs in 2019. Health Payer Intelligence. Accessed at https://healthpayerintelligence.com/news/large-employers-to-average-3.6m-on-wellness-programs-in-2019.
- Mattke, S. et al. 2014. ‘Workplace wellness programs: Services offered, participation and incentives.’ Rand Corporation.
- Blocker, T. February 13, 2016. ‘Why your employees aren’t participating in wellness programs.’ Wallace, Welch & Willingham. Accessed at: https://w3ins.com/news/why-your-employees-arent-participating-in-wellness-programs/
- Harvey, M. Can Technology Drive Engagement in Wellness Programs? Accessed at: https://hero-health.org/blog/can-technology-drive-engagement-in-wellness-programs/
- Ghose, A. et al. 2022. ‘Empowering patients using smart mobile health platforms: evidence of a randomized field experiment.’ Management Information Systems (MIS) Quarterly. 46:1.
- Hinge Health. 2021. ‘Survey Report: New Health Risks of the Remote Workplace.’ Accessed at: https://www.hingehealth.com/new-health-risks-of-the-remote-workplace/
- Pappas. C. September 24, 2019. ‘Top 20 eLearning statistics for 2019 you need to know.’ eLearning Industry. Accessed at: https://elearningindustry.com/top-elearning-statistics-2019
- Safety + Health Magazine. January 30, 2019. ‘Job seekers weigh health and wellness benefits during searches: survey.’ Accessed at https://www.safetyandhealthmagazine.com/articles/18009-job-seekers-weigh-health-and-wellness-benefits-during-searches-survey


