AI in occupational health is creating a lot of excitement and a lot of anxiety. Clinicians, occupational health teams, and industrial hygiene professionals are hearing about AI’s transformative potential from every direction. But the real question isn’t whether AI can do something impressive. It’s whether AI can solve the right problems.
The answer starts with understanding what’s happening on the ground.
The Workload Problem AI Can Actually Solve
The biggest challenge in occupational health today isn’t a technology problem. It’s a workload problem.
Clinicians and occupational health teams are spending more time documenting care than delivering it. Paper forms, manual data entry, charting after hours, piecing together information from multiple sources — the administrative weight is significant. And it’s not because professionals want to work this way. It’s because the system requires it.
The numbers tell the story. Clinicians can spend 50 to 70 percent of their day on documentation. For industrial hygiene professionals, the picture is similar. An estimated 60 to 70 percent of field records are captured on paper first, then re-entered into digital systems. That re-documentation takes more time than the IH work itself.
When AI handles the documentation burden, something interesting happens. Clinicians make more eye contact with patients. Patients share more. The quality of care improves not because the clinical judgment changed, but because the clinician is actually present in the conversation instead of staring at a screen.
Research supports this. A study published in JAMA Network Open found that after just 30 days of using AI-assisted documentation, providers reported a 13 percent drop in burnout and a meaningful increase in their ability to give patients undivided attention. The secondary benefits compound: less after-hours charting, higher job satisfaction, and more time spent on the work clinicians came into these roles to do: patient care.
That’s the case for AI in occupational health. Not innovation for the sake of innovation. The question is simply: can AI give clinicians and IH professionals their time back?
The Risks Are Real — and They Matter
Before rushing to adopt AI, occupational health professionals need to face the risks honestly. These are not theoretical concerns. This is patient data, worker health data, sensitive information, and clinical decisions.
The first concern is accuracy. AI systems can hallucinate: generating plausible-sounding information that is factually wrong. In occupational health, every record must be defensible. If an AI tool produces something a clinician cannot trace back to source data, that’s a serious problem. The questions that matter are: where did this information come from? Can it be verified? Can it be audited later?
Many consumer AI tools are simply not built for that level of traceability.
The second concern is human oversight. Occupational health professionals worry — rightly — that AI will start making clinical decisions, writing incident findings, or recommending actions without human review. That’s not just uncomfortable. It’s unsafe. AI in occupational health must assist professionals, not replace them.
The third concern is data privacy. Clinicians are trained to be extremely protective of patient data. The questions customers ask are direct: Where is my data going? Is it leaving my system? Is it being used to train public models? Who has access to it? In occupational health, data cannot be sent to a generic AI engine in the cloud. For most organizations, that’s a non-starter.
These risks — accuracy, auditability, privacy, and maintaining human control — are exactly the reasons many organizations are hesitant about AI. And they should be. How AI is built matters more than what AI can do.
What Responsible AI Looks Like in Occupational Health
The risks described above are real, but they’re addressable when AI is designed with occupational health requirements in mind from the start.
Data security in clinical environments demands more than standard enterprise protections. Cority’s Cortex AI applies the same data and applicability security standards embedded across the CorityOne platform, including security guardrails that prevent personally identifiable information (PII) and protected health information (PHI) from being shared with AI models. A zero data retention policy means data shared with an AI model to generate an output is never retained by that model. It cannot be used in other situations and cannot be used to train models available to other users.
Auditability is equally critical. For occupational health records to be defensible, every AI output needs to be observable. Cortex AI provides full visibility into data sources, prompts, models, and responses — with complete audit logs — so clinicians always know where an AI output originated and why. Every output requires human interaction and validation before it becomes part of the record. This human-in-the-loop design doesn’t just catch errors. It delivers the feedback necessary for improved AI accuracy over time.
Cority’s AI teams follow a foundational design principle when building the Cortex AI agents: if a user cannot execute an action, neither should the AI agent. This means AI permissions mirror the same role-based access controls that govern the platform. The AI cannot see, modify, or act on data that the user themselves wouldn’t have access to.
And unlike standalone AI tools that require clinicians to switch systems or learn new platforms, Cortex AI agents are embedded directly into existing CorityOne workflows. The AI assists right where professionals already work, reducing disruption and accelerating adoption.
Medical Scribe Agent: Giving Clinicians Time Back With Patients
In occupational health, documentation is essential. It’s how care is communicated, tracked, and measured. But for clinicians, documentation is one of the most time-consuming parts of their job.
Cortex AI’s Medical Scribe Agent takes this burden away. As clinicians focus on the patient, the agent listens in the background to capture the exchange, extracting the details that matter, filtering the noise, and presenting a clean summary the clinician can review in seconds.
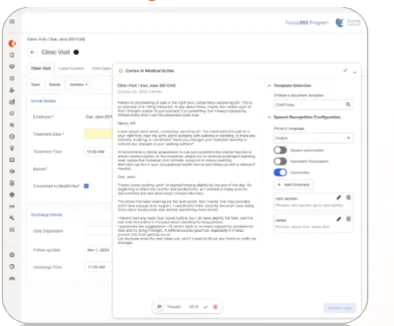
The Medical Scribe Agent is powered by a medical-grade language model designed specifically for healthcare. It’s built to understand clinical terminology, context, and sensitive patient data — ensuring precision and compliance while giving clinicians more time to focus on what matters most.
When implemented well, the results go beyond time savings. Note quality improves because the AI captures details clinicians might miss while multitasking. After-hours charting decreases. And clinicians remain fully in control of the final record: the scribe supports their thinking, preserves their voice in the note, and aligns with clinical and regulatory expectations.
Accuracy, context, and accountability matter more than speed. That’s why Cority invested in a medically trained model with the ability to learn and improve from clinician feedback over time.
Vaccination Record Scanning Agent: Paper to Digital in Seconds
While occupational health practices continue to digitize, there’s still a lot of paper. Stacks of handwritten notes, reports, and vaccination cards still need to make it into the system. Collecting accurate immunization history is critical, especially when running busy seasonal flu clinics or onboarding large groups of new hires.
Cortex AI’s Vaccination Record Scanning Agent eliminates the manual step. Clinicians snap a photo of an immunization record, and the AI reads the document, extracts the vaccine information, and enters it into the digital vaccination record. No manual transcription required.
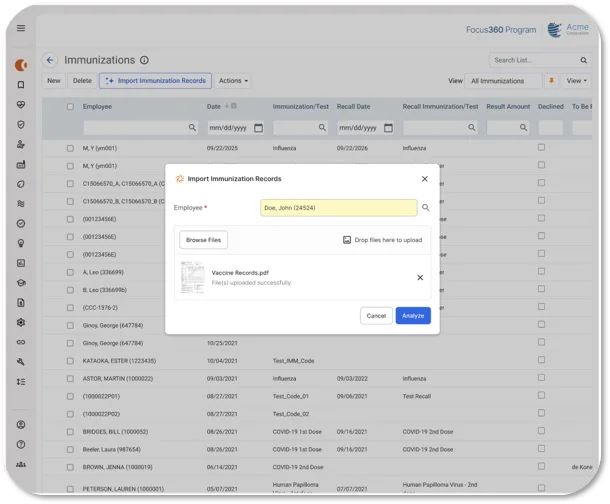
The result is fewer errors, cleaner health histories, and faster clinic throughput. Patients spend less time waiting, and clinicians spend less time typing.
Research supports the approach. A 2024 study published in PLoS ONE compared time and error rates for recording vital signs and prescriptions using manual entry versus OCR-based digitization. While results varied by data type, OCR consistently showed lower error rates than manual entry for both categories. The technology continues to improve.
The balance between automation and human review is built into the workflow. Clinicians always review and confirm before data becomes part of the record.
Questionnaire Scanning Agent: Eliminating Double Data Entry in Industrial Hygiene
Workplace inspections are a critical part of any effective EHS program. But in places like clean rooms, labs, and field environments where electronics can’t be used, inspections still happen on paper. The result is a familiar problem: IH professionals complete forms by hand in the field, then return to their desks to re-enter everything into the system.
Cortex AI’s Questionnaire Scanning Agent eliminates that double data entry. Professionals upload a photo of a handwritten inspection form, checklist, or survey, and the AI reads the document and transcribes the information directly into a digital record in CorityOne. All that’s needed is a review and confirmation. No re-entry, no lost details.
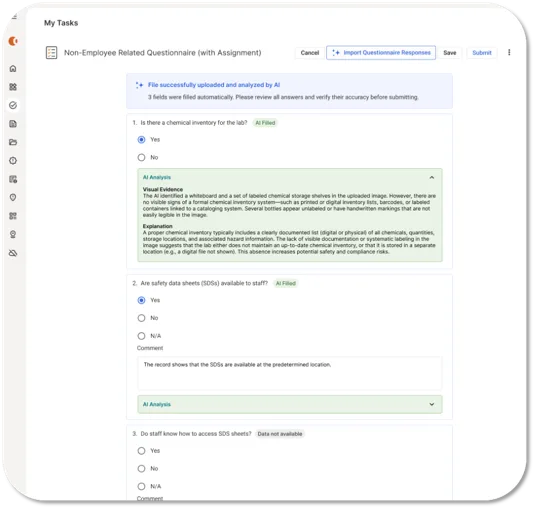
This agent turns paper records into measurable insights instantly. And the same approach — smart, contextual scanning that understands the structure of a form — can apply wherever organizations need to bridge the gap between field-based paper processes and digital record-keeping.
Where Most Organizations Stand Today
AI adoption in occupational health is still early. Most organizations fall into one of four stages: foundational (digitized records and rules-based alerts), predictive (risk stratification and demand forecasting), intelligent (clinical decision support and workflow automation), or adaptive (personalized care pathways and real-time learning systems).
The majority of organizations are in that first category or somewhere between exploration and early pilot mode. There’s a lot of executive interest and attention, but not always a clear roadmap for how AI fits into operational workflows.
That’s a reasonable place to be. The risks discussed earlier are real, and caution is warranted. But the key insight is this: AI adoption in occupational health doesn’t require a big transformation. It starts with small, safe, practical improvements to the work professionals are already doing: removing documentation time, digitizing paper records, and letting clinicians focus on patient care.
AI Is a Partner, Not a Replacement
AI in occupational health is here to stay. Practical use cases are already delivering value. The risks are real but manageable with the right design principles. And thoughtful adoption — starting with the administrative burden that consumes clinicians’ and IH professionals’ days — is what unlocks AI’s promise.
The goal was never to replace professional judgment. It’s to remove the typing, the transcription, and the rework so occupational health professionals can do more of what only they can do: assess, decide, and care for people.
For organizations exploring how AI fits into their occupational health programs, Cority’s Cortex AI is purpose-built for EHS workflows: secure, auditable, human-in-the-loop, and embedded in the systems teams already trust.
See how AI is also transforming workplace safety programs, or explore Cority’s Health solution set.




